What is Best Treatment for Arthritis in Lower Back?
 Myron
|
Myron
|
 02 Mar 2026
02 Mar 2026
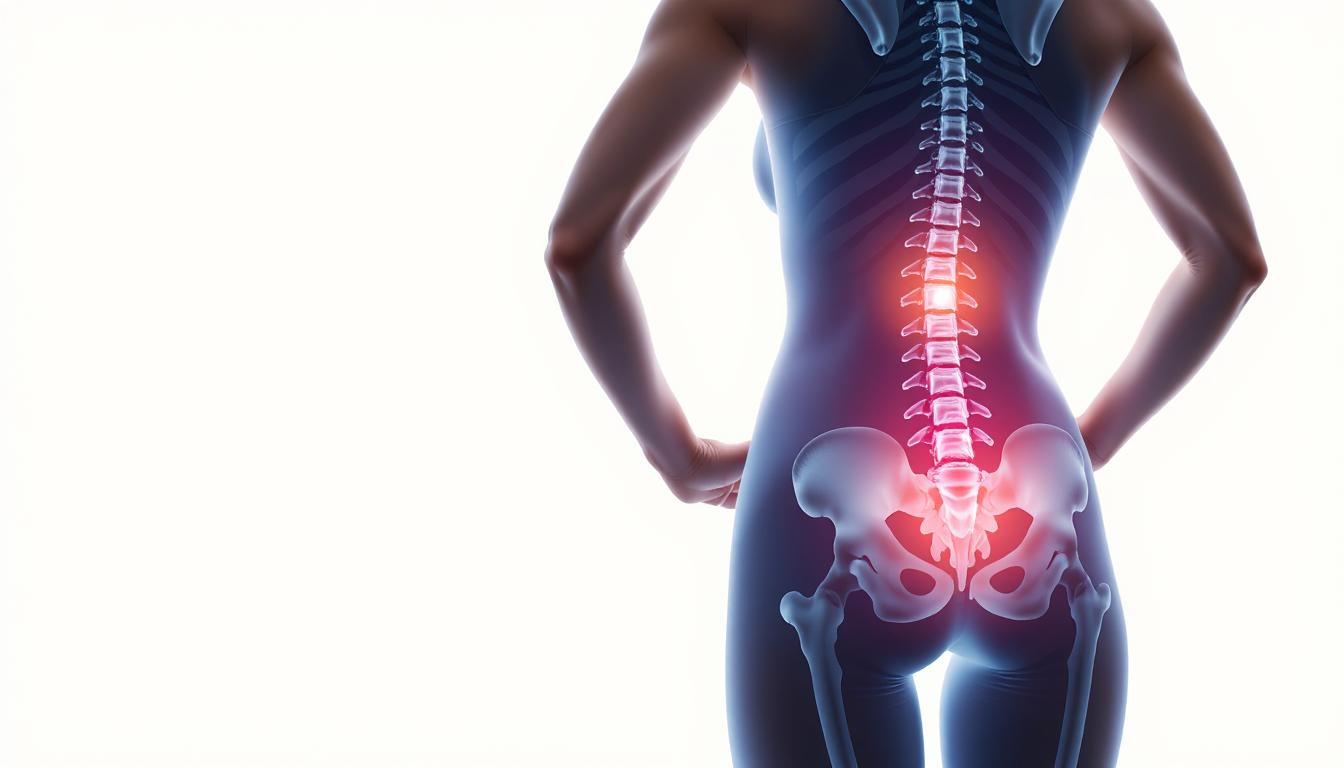
Understanding Lower Back Arthritis
Lower back arthritis is usually “wear and tear” in the joints of the lower spine. Most of the time, it’s osteoarthritis, sometimes mixed with degenerative disc disease. People often imagine one “bad disc,” but a lot of the pain comes from small joints in the back of the spine called facet joints. Those joints are like hinges. They let you bend and twist. Over years, the smooth lining (cartilage) can thin out. When that cushion is thinner, the joint gets irritated more easily. That irritation shows up as stiffness, aching, and sometimes a sharp catch when you move a certain way.
So the best treatment for arthritis in lower back is rarely one magic thing. It’s usually a few pieces done consistently: moving more (but the right kind), building support muscles, managing flare-ups, and using medicine carefully when needed. That’s the core of good lower back arthritis treatment.
Common symptoms of lower back Arthritis
Lower back arthritis tends to feel predictable. Not always, but often.
Common symptoms:
-
A dull ache in the low back that sticks around
-
Stiffness when you get out of bed or after sitting
-
Pain that ramps up with prolonged standing, bending, or repeated lifting
-
Feeling “tight” or less flexible through the day
-
Some people feel better once they warm up, then worse again after too much activity
Arthritis pain is often worse at the end of a long day. Muscle strain is often worse right after one incident. That difference isn’t perfect, but it helps people understand what’s going on.
If pain shoots down the leg, that can still happen with arthritis, but it often means a nerve is irritated too. That’s when you start thinking about a medical evaluation sooner.
First-line treatment: lifestyle modifications
If you look at how to treat arthritis in lower back, this is where most people start, and honestly where most improvement happens.
Weight (if relevant):
Extra weight isn’t “the cause” of arthritis, but it does increase load. The lower back is a load-bearing area. Even a small reduction can reduce daily stress on joints.
Sitting less, breaking it up:
Long sitting compresses the low back and tightens hip flexors. Even if you have a desk job, try a pattern like:
-
stand up every 30–60 minutes
-
walk for 1–2 minutes
-
do a gentle back bend or hip stretch (nothing aggressive)
Posture and ergonomics:
This doesn’t mean “sit perfectly straight all day.” That’s tiring. It means reduce obvious strain:
-
feet flat
-
screen at eye level
-
lower back supported
-
avoid leaning forward with your head/neck for long periods
Daily movement habit:
Arthritic joints generally hate two things: too much load, and too much stillness. Gentle movement is like oil for a hinge. You’re trying to keep the hinge moving without forcing it.
These are boring steps, but they’re often the foundation of lumbar spine arthritis pain management.
Physical Therapy
If you want a “superhuman” explanation, here’s the simple truth: the spine is not meant to be held up by bones and joints alone. It’s meant to be supported by muscle.
Physical therapy for lumbar arthritis usually targets:
-
Core strength (front and sides of abdomen)
-
Glutes and hips (huge for taking load off the low back)
-
Small stabilizers around the spine
-
Flexibility in hips and hamstrings (tight hips make the low back do extra work)
A good PT program isn’t just “do these exercises.” It teaches:
-
How to hinge at the hips instead of rounding the lower back
-
How to get up from a chair without twisting poorly
-
How to lift and carry without loading irritated joints
A lot of people feel pain relief from PT not because arthritis disappears, but because the joints are no longer taking the full hit of every movement.
Heat and cold therapy
These sound too simple, but they help many people.
Heat is usually better for stiffness:
-
morning stiffness
-
tight muscles
-
“I feel locked up”
Heat relaxes muscle guarding. When your back hurts, muscles tighten to protect you. Heat helps those muscles let go.
Cold is often better for flare-ups:
-
after you overdid activity
-
swelling-type soreness
-
hot, irritated feeling
If you’re not sure:
-
heat before activity to loosen
-
cold after activity if it’s irritated
This fits under natural remedies for lower back arthritis that are safe and practical.
Over-the-counter pain relief
For many people, OTC options are part of medicine for lower back arthritis, especially during flare days.
-
Acetaminophen can help pain but doesn’t reduce inflammation. It’s sometimes a good first step for mild pain.
-
NSAIDs like ibuprofen or naproxen help pain and inflammation. They can be useful if inflammation is a big part of your flare.
Important cautions (because this matters):
-
NSAIDs can irritate the stomach and raise bleeding risk
-
they can affect kidneys
-
they can raise blood pressure in some people
-
they interact with certain blood thinners and other meds
Topical gels/creams (like anti-inflammatory gels) can help if pain feels superficial or localized. They won’t “fix” arthritis, but they can take the edge off without as much whole-body exposure.
If you’re unsure what is safe with your health conditions and current meds, Sanford Pharmacy can review what you’re taking and help you choose an option that fits your situation.
Prescription medications
Prescription options vary because not every back pain pattern is the same.
Depending on the situation, a clinician might consider:
-
stronger anti-inflammatory meds for a short period
-
muscle relaxants if muscle spasm is a major feature (usually short-term)
-
nerve pain medicines if there’s nerve irritation (more leg symptoms)
-
limited short-term pain meds in select cases (not a long-term plan)
Corticosteroid injections can be helpful in certain cases:
-
facet injections (if the facet joints are confirmed pain source)
-
epidural steroid injections (more for nerve irritation)
Injections can reduce inflammation and calm a flare, but they don’t rebuild cartilage. They are usually used to create a window where you can move better and build strength.
Exercise and movement programs
This is where many people either get better or get stuck. Because doing nothing feels safe, but it often makes arthritis worse long term.
The best exercises for arthritis in lower back are usually low-impact and repeatable:
Walking
-
simple
-
adjustable (10 minutes counts)
-
improves blood flow and keeps joints moving
Swimming or water walking
-
water supports body weight
-
movement without heavy load
-
great for people who flare with land exercise
Core work (gentle, controlled)
-
dead bug variations
-
bird dog
-
side planks (modified)
These teach the trunk to stabilize without forcing painful ranges.
Hip and glute strengthening
-
bridges
-
clamshells
-
step-ups (small step)
Strong hips reduce how much the low back has to “do everything.”
Stretching
-
hip flexor stretch
-
hamstring stretch (gentle)
-
piriformis/hip stretch
This reduces pull on the low back.
The key is consistency. Ten minutes daily beats one intense workout once a week. If you want long-term improvement, this is often the biggest part of lower back osteoarthritis treatment.
Advanced treatment options
If conservative care fails, there are other options. These are typically considered after a solid attempt at PT, exercise, and medication management.
-
Epidural steroid injections (more nerve-related pain)
-
Nerve blocks (can help confirm pain source)
-
Radiofrequency ablation in some cases (targets pain signals from certain facet joints)
Surgery is usually not the first answer for arthritis-only pain. It may be considered if there’s a severe structural issue, progressive nerve deficits, or pain that does not respond to well-done conservative care.
These fall under lumbar arthritis treatment options beyond the basics.
When to seek medical evaluation
Get checked sooner (not later) if you have:
-
pain radiating down the leg with numbness or weakness
-
worsening weakness in the foot/leg
-
numbness in the groin/saddle area
-
loss of bladder or bowel control (emergency)
-
fever with back pain, or unexplained weight loss
-
pain after a major fall/trauma
Also get evaluated if:
-
symptoms are not improving after a few weeks of consistent conservative care
-
pain is steadily worsening
-
you can’t function day to day
Role of ongoing support
Most people do best when they treat this like a long-term condition with a plan, not a one-time crisis.
Helpful ongoing steps:
-
periodic check-ins with a clinician
-
keeping an exercise routine even when you feel better
-
using meds only as needed and safely
-
learning your flare triggers (standing too long, long car rides, heavy lifting, poor sleep)
Sanford Pharmacy can help with:
-
picking an appropriate OTC option (acetaminophen vs NSAID vs topical)
-
checking interactions with your current medicines
-
helping you use pain relief products safely (heat wraps, topical gels, supports)
Categories
Can Recurrent Utis Be a Sign of Cancer
 Jose
Jose
How Does Hydroxychloroquine Work?
 Ali
Ali
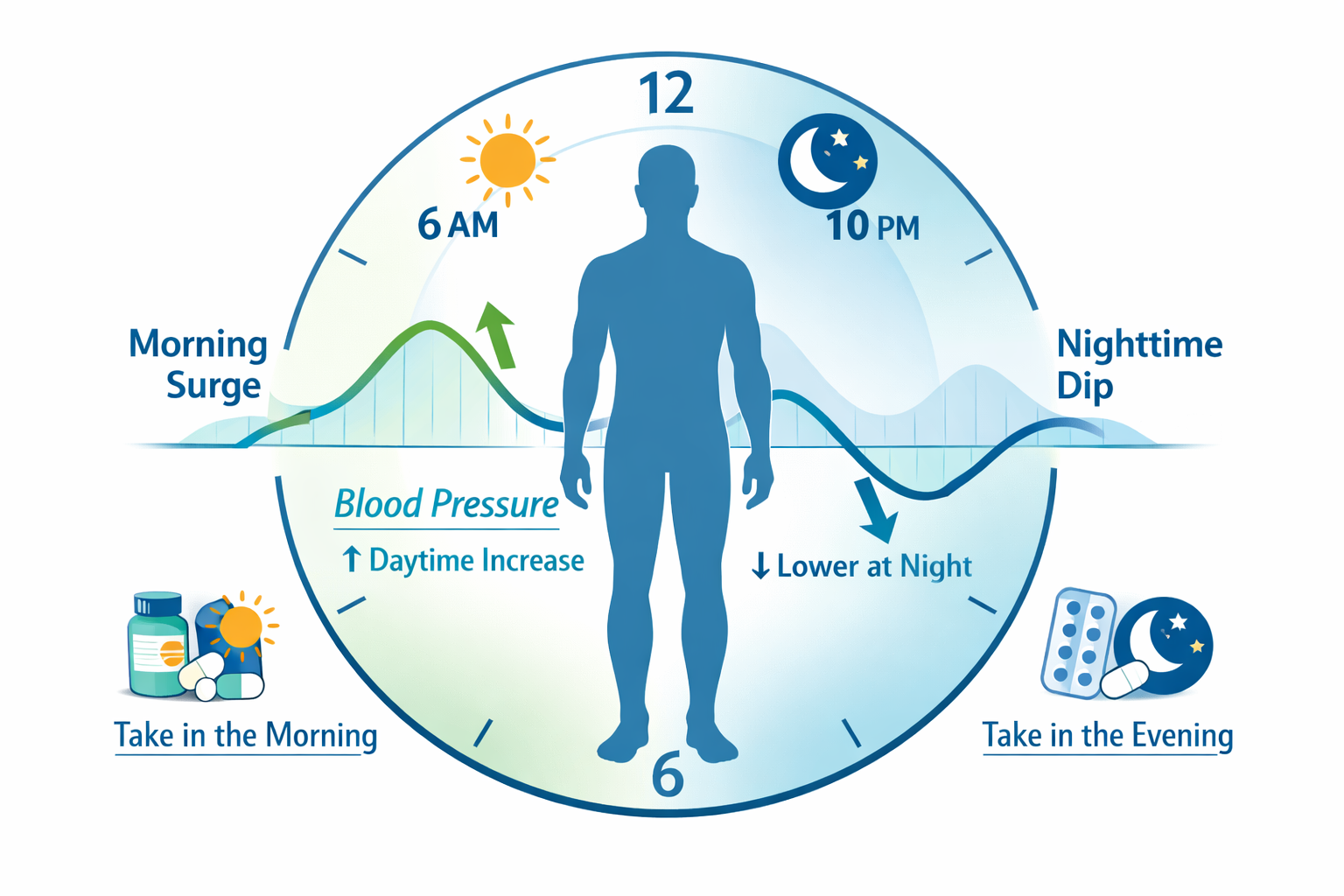
Morning vs Night: Optimizing Blood Pressure Medication Timing
 Arely
Arely
Natural Thyroid Hormone Therapy for Hypothyroidism Explained
 Dulce
Dulce
What Is Raloxifene Used For?
 Abdullah
Abdullah










.webp)
.webp)
-(2).webp)
.webp)